Stenosis is a Greek term which means "narrowing". Imagine a narrowing in a water way, like a river, where the river narrows and flow is restricted. This representation is similar to what stenosis looks like inside the spinal canal. Anything can cause the narrowing, but in the lumbar spine, the most likely causes are bony overgrowth, thickened ligamentum flavum, a disc herniation, or some combination of these.
Symptoms of Stenosis in the Lumbar Spine
The problem stenosis causes is nerve compression. The incidence of problems certainly increases with age, and the symptoms can take decades to manifest. The nerves in the spinal canal are not very sensitive to slow increases of pressure, so the stenosis or bony encroachment in the central canal can occur over a period of decades without any symptoms. Sometimes people will come into the office, after three to six months of symptoms, even though the stenosis is severe and has been developing for years.
This is very different from the pain from a disc herniation which happens abruptly and causes much more acute pain. The disc herniation causes stenosis too, but stenosis usually refers to the bony overgrowth in the spine that causes symptoms to occur more slowly. So slowly that you can even see people’s posture changing to accommodate the problem. Here are a few of the symptoms:
Positive shopping cart sign
This is a “leaning forward” posture change that can occur with stenosis. It is unconscious and so common that it has a name, a “positive shopping-cart sign”. If you go to the grocery store or Home Depot and like to get a cart so you can lean forward, this is referred to as a positive shopping-cart sign. The reason that people like to lean forward is because it reduces the pressure on the cauda equina. The posture changes to reduce the pressure on the nerves which reduces the pain
Pain or numbness in legs, thighs, calves, or buttocks.
Typically, the pain is in one or more of these areas. You can have back pain, buttock pain, thigh and leg pain, or foot pain. If you experience numbness it’s usually in the thighs, calves or buttocks.
Pain while walking
One activity that causes pain is walking any distance. Walking endurance can be significantly reduced from a few blocks to a few hundred feet. As endurance decreases with time, it might become necessary to sit down and rest when walking even short distances. Sitting down for a few minutes will relieve the symptoms of thigh and leg pain until you can get back up and start walking again.
Diagnosis
Diagnosis is made by understanding the patients medical history, and taking a look at their symptoms and physical examination. Typically imaging is used to accurately assess the issue. MRI, CAT scan, X-ray, or a myelogram may be used, although the MRI is the best way to look at the interior of the spine.
The images clearly show the bone, discs, ligamentum flavum and nerves in the spinal canal. The MRI takes slices in different planes to give a 3-dimensional look at the interior of the spinal canal. Areas of tightness or stenosis can be seen and measured. We can look inside the central canal and see where the stenosis is located and what is causing the tightness. The MRI scan gives two views of the spine, the sagittal view and the axial view. The views are shown in multiple slices and the sagittal and axial views can be correlated on the computer.
Anatomy of the Lumbar Spine
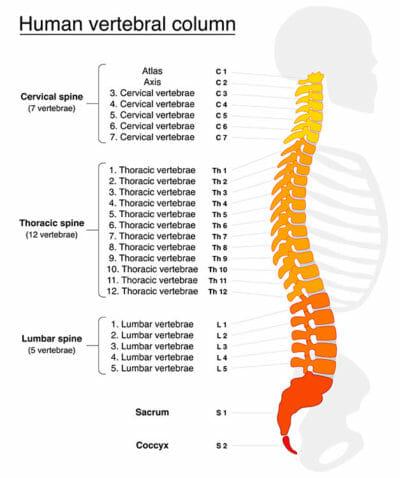
The spinal cord really ends at the lumbar 1 vertebrae. Beyond that, the nerves separate and continue down to the sacrum as separate nerves. The separated nerves beyond the lumbar 1 vertebrae are called the cauda equina, which means “horse’s tail” since that is what they look like when they spread out after separating from the spinal cord. The nerves of the cauda equina travel inside of the main or central spinal canal until they exit through the foraminal canals and go out to the buttock, thigh, leg and feet.
Where Does Spinal Stenosis Occur in the Lumbar spine ?
Spinal stenosis in the lumbar spine can occur in two locations: One is inside the large canal which is the central canal. Two, stenosis can also occur in the foraminal canals, which are the little side channels where the nerves actually take a pathway out of the central canal. This article will only discuss central canal stenosis.
What Causes Spinal Stenosis ?
Spinal stenosis is the result of degenerative changes to parts of the spinal column. Degenerative changes can occur over a number of years and act to change the dimensions of the spinal canal. These changes can be considered developmental, but can be aggravated or accelerated by any congenital narrowing of the spinal canal.
The causes are often a combination of wear and tear and gravitational forces, that tend to compress and narrow the disc spaces. As the facet joints collapse, they degenerate and overgrow into the spinal canal. An analogy would be degenerative finger joints in an older person. You may have seen the bone overgrow to the point of having to resize the rings. The facet joints in the back are similar to the finger joints in that when they overgrow, they grow into the spinal canal and compete for space with the nerves of the cauda equina.
The result is a space issue as narrowing of the spinal canal occurs. Think of an old metal water pipe with calcium deposits on the inside occurring over a number of years, with the result being loss of water flow. This narrowing or stenosis is well shown on the MRI’s sagittal and axial views.
In addition to the bone, there is a thick soft tissue that lines the spinal canal and covers the cauda equina. It is called the ligamentum flavum (yellow ligament) and it can actually buckle over itself with collapse and loss of the disc height. The buckling of the ligamentum can be a big contributor to the spinal stenosis. The end result is facet overgrowth and ligament buckling that grow into the spinal canal and compress the cauda equina, or all the nerves that go to your thighs, legs, and feet.
Treatment for Spinal Stenosis
As said above, compression is the problem so the obvious treatment is decompression.
My recommendation to treat spinal stenosis of the lumbar spine, is to endoscopically decompress it, without a fusion unless there is a lot of deformity, which is rare. You may want to read an article I wrote on why you should avoid a fusion.
Endoscopic procedures are referred to as being “minimally invasive”, which is a term with a lot of confusion around it. It’s confusing because it doesn’t mean anything; it is not well defined. The typical tube size of minimally invasive tubes, is usually 18 to 24 mm. Compare that to the endoscopic tube sizes of 8 or 10 mm. Endoscopic surgery is currently the ultimate in minimally invasive. So the term “endoscopic” does mean something.
Endoscopic spine surgery almost always refers to decompression without a fusion using a ½-inch incision or less. Compare open surgery to this that uses a 3” to 7” incision with significant soft tissue stripping
There are two ways to decompress. One approach is to decompress indirectly and the other is to decompress directly.
The most common way to decompress indirectly is the epidural steroid injection. When the epidural steroid is injected into the spinal canal, the powerful anti-inflammatory effects of the steroid actually shrink the nerves a little. The shrinking creates more space indirectly and is usually short acting.
Another way to decompress indirectly is to open the spinal canal with a mechanical device placed between the spinous processes an example of such a device is a CoFlex implant. The CoFlex device is spring loaded and jacks the disc space open, creating some additional space inside the spinal canal.
Request your Free Consultation
How do we decompress directly ?
Direct decompression is accomplished with some bone removal giving the cauda equina nerves some additional space. This bone removal is referred to as a laminotomy if some of the lamina is removed and a laminectomy if the entire lamina has been removed. The lamina is the bony covering of the spinal canal on the back or posterior side.
In addition to removal of the bone, there is a very thick ligament that lines the spinal canal that must be removed as well. This thick ligament is called the ligamentum flavum and feels like hard rubber. Both bone and ligament need to be removed to some extent to decompress adequately.
How much bone and ligament has to be removed ?
The simple answer is “enough to decompress the spinal nerves”, but not enough to destabilize the spine. When one looks at the area of stenosis on an MRI, the areas of stenosis are usually not extensive, maybe a centimeter or a little more, not that much.
The surgery can be accomplished with a 7-mm tube which is small enough for minimal disturbance to the surrounding soft tissues but large enough to pass the instruments needed to effectively decompress the cauda equina. The precision of the German tools allows removal of a portion of the lamina but not the entire lamina. If you remove too much bone, you can have instability issues, particularly if a large amount of the facet joint is taken.
Is there something that you don’t want to remove during surgery ?
Yes, the soft tissues that contribute to stability. Stability is maintained by two components, the bone and the soft tissues. The soft tissues are oftentimes under appreciated. For example, think of a sailboat with a lot of wind coming across the sail. The only reason that the mast stays upright is because of the ropes and stays that support it. If you divide the ropes and stays that hold the mast up, the mast may become unstable and will break. It is the same in the back. You have to have the soft tissue attachments to help stability. Lack of stability will head you in the direction of a fusion.
There are similar clinical outcomes whether you decompress with or without a fusion. This is why I do not recommend starting with a fusion, there are more complications both short term and long term with a fusion.
What about complications ?
Let’s talk about fusion complications: Short term, infection rate is 1%, re-operation 4%. Long-term adjacent disc disease occurs at a rate of 5% per year afterward. So, if you are 10 years out, there is a 50% chance you are going to have some adjacent disc disease or degenerative changes. It does not mean you are going to have to have an additional surgery, but it is certainly heading in that direction. If you look at the long-term complications from all causes, it is 6% to 11%. So, we have hardware in place that you cannot really take out if you do not like it; there is not much you can do about it.
How about complications of decompression without a fusion ? The infection rate is less than 0.1 %. Reoperation is less than 1%. Long-term issues: No adjacent disc disease, no non-unions, no hardware issues.
When I look at these figures, I would do the endoscopic decompression first; and if it is not successful, you can always do a fusion with hardware.